Carotid stenosis is narrowing of the carotid arteries. This is usually due to atherosclerotic disease present in the internal carotid arteries.
The internal carotid arteries supply a significant portion of the brain with blood, nutrients, and oxygen. If carotid stenosis is present it can result in transient ischemic attacks and possibly stroke.
Signs and Symptoms
Carotid stenosis may be either symptomatic or asymptomatic. Symptomatic carotid stenosis presents in one of three ways: transient ischemic attacks, stroke, or amaurosis fugax.
Transient ischemic attacks (TIA) occur when blood to the brain is blocked temporarily. TIAs cause the same symptoms as a stroke, but the symptoms resolve over 24 hours and there is no permanent brain injury.
A sub-category of TIA is a symptom known as amaurosis fugax, which is a temporary loss in vision, usually in one eye. It is described by patients as a curtain being drawn over the affected eye. It is caused by a small blood clot that breaks off from an atherosclerotic plaque present in the internal carotid artery. This small clot enters the retinal artery and occludes blood flow causing temporary blindness.
Stroke is by far the scariest problem associated with carotid stenosis. When a stroke occurs it can cause severe and irreversible brain injury. Strokes can cause life changing symptoms such as paralysis, aphasia (inability to speak or understand language), and even death!
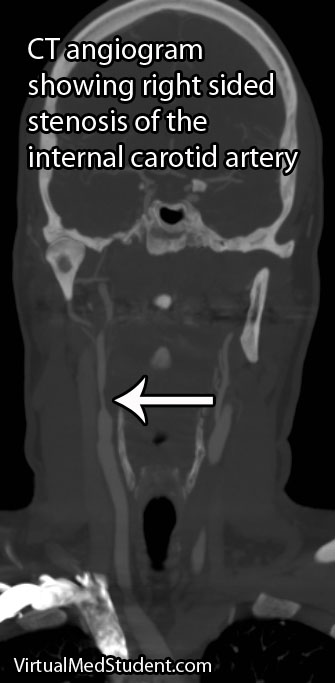
Diagnosis
Diagnosis of carotid stenosis is based on imaging studies. The most commonly employed studies are carotid ultrasound, CT angiogram, MR angiogram, and formal angiography.
Treatment
Treatment is dependent on the location and degree of stenosis. Lesions that are near the origin of the internal carotid artery are frequently fixed with surgery in a procedure known as an endarterectomy. In a carotid endarterectomy the artery is surgically opened and the atherosclerotic material is "scooped" out.
The benefit of carotid endarterectomy on stroke risk for symptomatic patients is dependent on the degree of narrowing in the vessel. A landmark study in 1991 showed that carotid endarterectomy was very beneficial in preventing stroke in already symptomatic patients when the degree of narrowing was high (defined as 70 to 99%). A different study looked at lesser degrees of stenosis (50 to 69%) and found a benefit, albeit less robust. There is no clear benefit to having surgery in patients who have narrowing that is 50% or less. Surgery in asymptomatic patients with higher degrees of stenosis follows a more complicated algorithm.
If the diseased segment is higher up on the internal carotid, and surgical access is anatomically difficult, then procedures like carotid stenting or angioplasty can be performed. Stenting is a procedure in which a tiny metal tube-like device is threaded up through the femoral artery in the groin and then opened to “re-expand” the diseased arterial segment.
Patients who may not tolerate a procedure are often managed medically with antiplatelet medications such as aspirin, aspirin/dipyridamole combo (Aggrenox®), ticlopidine (Ticlid®) or clopidogrel (Plavix®). Currently there is no "best" medication to prescribe; the choice is highly dependent on the individual patient and physician.
Overview
Carotid stenosis refers to narrowing of the internal carotid artery. It is usually due to atherosclerotic disease. It can cause transient ischemic attacks, stroke, and amaurosis fugax. Diagnosis is with CT angiogram, carotid ultrasound, and/or formal invasive angiography. Treatment is highly variable, but usually involves a combination of surgery (endarterectomy), stenting, angioplasty, and antiplatelet medications like aspirin.
References and Resources
- Barnett HJ, Taylor DW, Eliasziw M, et al. Benefit of carotid endarterectomy in patients with symptomatic moderate or severe stenosis. North American Symptomatic Carotid Endarterectomy Trial Collaborators. N Engl J Med. 1998 Nov 12;339(20):1415-25.
- Chambers BR, Donnan GA. Carotid endarterectomy for asymptomatic carotid stenosis. Cochrane Database Syst Rev. 2005 Oct 19;(4):CD001923.
- [No authors listed]. Beneficial effect of carotid endarterectomy in symptomatic patients wth high-grade carotid stenosis. North American symptomatic carotid endarterectomy trial collaborators. N Eng J Med. 1991 Aug 15;325(7):445-53.
- Biller J, Feinberg WM, Castaldo JE, et al. Guidelines for carotid endarterectomy: a statement for healthcare professionals from a Special Writing Group of the Stroke Council, American Heart Association. Circulation. 1998 Feb 10;97(5):501-9.