Polycystic ovarian syndrome (PCOS) is a well recognized disorder of androgen excess in females. The pathology behind this disorder is a cyclic process related to obesity and hormone excess.
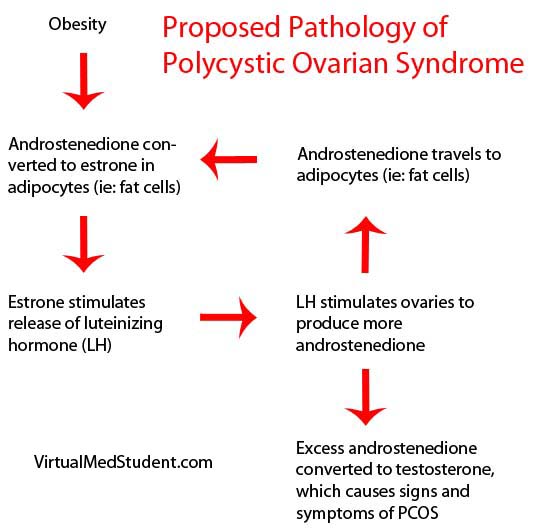
The cycle begins when luteinizing hormone from the pituitary gland stimulates the ovaries to produce an androgen known as androstenedione. Androstenedione travels in the blood stream to adipocytes (ie: fat cells) where it gets converted to a specific estrogen called estrone. Estrone then travels in the blood stream to the pituitary gland where it stimulates the release of more luteinizing hormone.
The excess luteinizing hormone stimulates the ovaries to produce more androstenedione. At this point, some of the excess androstenedione gets converted to testosterone, which causes the signs and symptoms of polycystic ovarian syndrome; the rest of the androstenedione gets converted to estrone in fat cells which further fuels the cycle.
Signs and Symptoms
The signs of polycystic ovarian syndrome are related to excessive estrogens and androgens. Excess androgens can cause hirsuitism (ie: growth of facial hair), acne, and oligo- or amenorrhea (ie: decreased frequency or lack of menstrual cycles, respectively). If severe enough, some women may have deepening of the voice and male-like balding patterns.
In addition, the elevated estrogen levels (ie: estrone) stimulate the proliferation of endometrial tissue resulting in abnormal uterine bleeding. If this occurs for a long enough period of time the patient is at risk for endometrial carcinoma.
Patients with polycystic ovarian syndrome are also at risk for other metabolic and cardiovascular diseases. Some patients develop diabetes mellitus, hypercholesterolemia, and hypertension. A substantial portion of patients also have co-existent metabolic syndrome.
Diagnosis
Diagnosis is made when at least two of the following three criteria are met:
(1) Oligo- or anovulation (ie: decreased frequency or lack of ovulation)
(2) Blood tests consistent with elevated androgen levels
(3) Polycystic ovaries seen on pelvic ultrasound
The name polycystic ovarian syndrome is somewhat of a misnomer because you do not need to have polycystic ovaries to be diagnosed with PCOS!
In addition laboratory data that supports the diagnosis of polycystic ovarian syndrome is an increased luteinizing hormone to follicle stimulating hormone ratio (increased LH:FSH), estrone levels greater than estradiol levels, as well as elevated androstenedione and/or testosterone levels.
Treatment
Treatment of polycystic ovarian syndrome is with birth control pills (oral contraception). The birth control pill decreases the release of luteinizing hormone by the pituitary, and breaks the cyclic pathology illustrated above.
In women who wish to become pregnant a medication known as clomiphene may be used. It is an anti-estrogen that ultimately causes an increased release of follicle stimulating hormone by the pituitary. The resulting increase in follicular development in the ovaries increases the odds of successful ovulation. Interestingly, an anti-diabetes medication known as metformin also increases the rates of ovulation and pregnancy in PCOS patients.
Since many patients also have metabolic syndrome it is important to begin treatments as necessary to control co-morbid conditions. Obese women should be encouraged to lose weight. Patient’s with diabetes and insulin insensitivity should be started on metformin. Patients with hypercholesterolemia may benefit from statin therapy.
Overview
Polycystic ovarian syndrome has a cyclic pathology related to obesity and elevated hormones. It causes masculinization with symptoms and signs like increased facial hair growth, balding, and lack of ovulation. Patients are also at risk for developing diabetes and other stigmata of the metabolic syndrome. Diagnosis is based on a combination of elevated androgens, polycystic ovaries, and abnormal menstrual cycles. Treatment is usually with oral contraception, although in women who wish to conceive, medications like clomiphene may be used.
References and Resources
- Teede H, Deeks A, Moran L. Polycystic ovary syndrome: a complex condition with psychological, reproductive and metabolic manifestations that impacts on health across the lifespan. BMC Med. 2010 Jun 30;8:41.
- Tang T, Lord JM, Norman RJ, et al. Insulin-sensitising drugs (metformin, rosiglitazone, pioglitazone, D-chiro-inositol) for women with polycystic ovary syndrome, oligo amenorrhoea and subfertility. Cochrane Database Syst Rev. 2010 Jan 20;(1):CD003053.
- Lujan ME, Chizen DR, Pierson RA. Diagnostic criteria for polycystic ovary syndrome: pitfalls and controversies. J Obstet Gynaecol Can. 2008 Aug;30(8):671-9.
- Beckmann CRB, Ling FW, Smith RP, et al.Obstetrics and Gynecology
. Fifth Edition. Philadelphia: Lippincott Williams and Wilkins, 2006.
- Bickley LS, Szilagyi PG. Bates’ Guide to Physical Examination and History Taking
. Ninth Edition. New York: Lippincott Williams and Wilkins, 2007.
- First Aid USMLE Step 1
Le T, Bhushan V, Grimm L. First Aid for the USMLE Step 1
. New York: McGraw Hill, 2009.