Hydrocephalus literally means "water head". It is a term used to describe a pathological increase in the amount of cerebrospinal fluid (CSF) within the ventricles (fluid filled cavities) of the brain.
In order to understand hydrocephalus we have to first appreciate the cerebrospinal fluid pathway and ventricular system of the brain. The brain has four ventricles: a pair of lateral ventricles, a third ventricle, and a fourth ventricle. They are connected to one another through narrow channels. The fourth ventricle drains into the subarachnoid space around the upper spinal cord. The spinal fluid travels down into the lumbar cistern and then back up again where it is absorbed by the arachnoid granulations overlying the cerebral hemispheres.
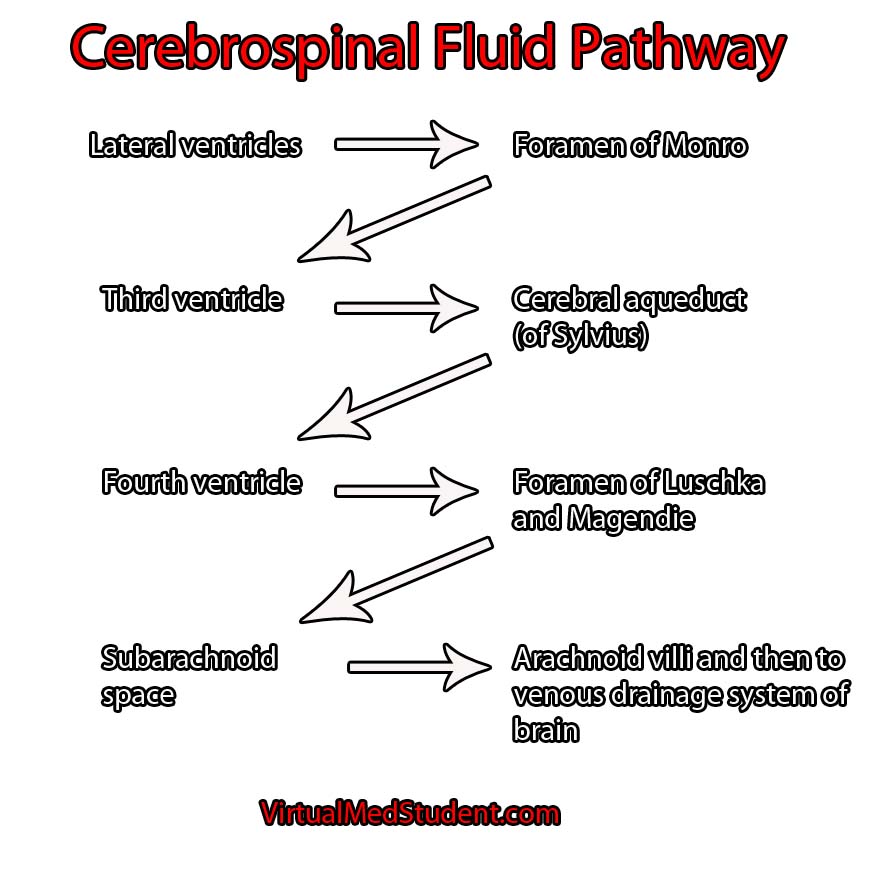
Cerebrospinal fluid is created at a rate of roughly 500 mL per day. It is primarily secreted by specialized cells within the walls of the ventricles known as choroid plexus. As you can imagine, if it is secreted at 500 mL per day there must be an equal amount of re-absorption. This re-absorption occurs in the subarachnoid space by venous structures known as "arachnoid villi". Re-absorption does not occur in the ventricles themselves; this is an important point to keep in mind as we discuss the difference between communicating and non-communicating forms of the disease.
Hydrocephalus occurs when excess cerebrospinal fluid backs up. It is called "communicating" hydrocephalus if all of the ventricles are enlarged. Otherwise it is known as "non-communicating" hydrocephalus. There is another informal type of hydrocephalus that is known as "ex-vacuo"; it occurs when dilation of the ventricular system is a result of brain tissue loss, rather than a pathological increase in the amount of cerebrospinal fluid.
The term hydrocephalus usually implies an abnormally high pressure within the ventricular system. However, a different type of hydrocephalus known as "normal pressure" hydrocephalus defies this rule.
Communicating hydrocephalus usually develops when the arachnoid villi get "gunked up". Abnormal materials (such as blood in subarachnoid hemorrhage or proteins after meningitis) can block the arachnoid villi and prevent re-absorption. The cerebrospinal fluid then backs up and causes the entire ventricular system to enlarge.
Non-communicating hydrocephalus is slightly different because the re-absorption pathway is functioning properly, but CSF backs up behind a "road block" in one of the channels connecting the individual ventricles. "Road blocks" can be anything from tumors to developmental narrowing of the channel itself. For example, colloid cysts of the third ventricle can occlude the foramen of Monroe (the channel between the lateral and third ventricles); when this occurs CSF produced in the lateral ventricles is not able to flow into the third ventricle. CSF then backs up in the lateral ventricle(s) resulting in pathologic dilation.
Overall, there are crap tons of causes for both communicating and non-communicating hydrocephalus. Some patients have congenital forms secondary to improper development of the CSF pathways. Others may develop hydrocephalus later in life as a result of infection, tumor formation, or aneurysm rupture.
Signs and Symptoms
The signs and symptoms depend on the age of the patient and the rapidity of onset. In newborns hydrocephalus often presents as failure to thrive with an abnormally enlarging head.
If hydrocephalus develops rapidly, the increase in intracranial pressure (as a result of cerebrospinal fluid putting pressure on the brain) leads to nausea, vomiting, headache, and if severe enough, coma and potentially death!
Normal pressure hydrocephalus (NPH) is a unique type of hydrocephalus in which there is no elevation in pressure (hence the term "normal pressure"). The classic symptoms of NPH are difficulty walking, dementia, and urinary incontinence.
Diagnosis
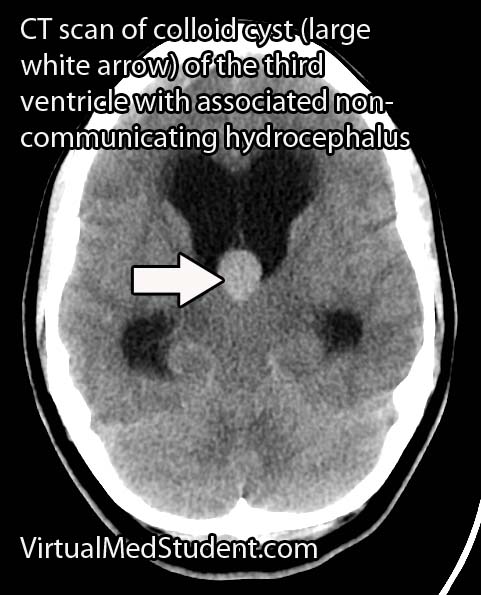
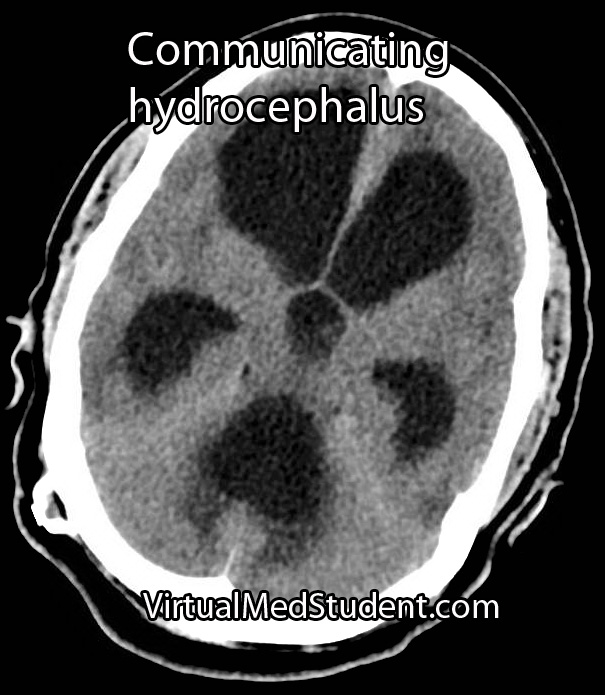
Diagnosis of hydrocephalus is made with CT scan coupled with clinical evidence of increased pressure within the ventricular system.
The scan will show an abnormally enlarged ventricular system. MRI scans with contrast are also routinely done to evaluate for tumors as a cause of hydrocephalus.
Treatment
Treatment consists of "shunting" the cerebrospinal fluid to another part of the body, usually the peritoneal cavity.
Other techniques such as third ventriculostomy, in which a surgically made "hole" is placed between the third ventricle and the subarachnoid space is also sometimes employed. This is very effective in cases of non-communicating hydrocephalus secondary to aqueductal stenosis (ie: the small passage between the third and fourth ventricles).
The ultimate treatment depends on the type of hydrocephalus and whether symptoms are severe enough to warrant surgical intervention.
Overview
Hydrocephalus is a pathological accumulation of cerebrospinal fluid. It can be communicating, non-communicating, or normal pressure. It can cause numerous signs and symptoms, but headache, nausea and vomiting are amongst the most common. Diagnosis is with CT scanning and clinical evidence of increased intracranial pressure. Treatment consists of shunting the CSF to another part of the body where it can be reabsorbed.
Related Articles
References and Resources
- Moorthy RK, Rajshekhar V. “Endoscopic third ventriculostomy for hydrocephalus: a review of indications, outcomes, and complications. Neurol India. 2011 Nov-Dec;59(6):848-54. Review.
- Factora R, Luciano M. “Normal pressure hydrocephalus: diagnosis and new approaches to treatment. Clin Geriatr Med. 2006 Aug;22(3):645-57.
- Chatterjee S, Chatterjee U. Overview of post-infective hydrocephalus. Childs Nerv Syst. 2011 Oct;27(10):1693-8.
- Cinalli G, Spennato P, Nastro A, et al. Hydrocephalus in aqueductal stenosis. Childs Nerv Syst. 2011 Oct;27(10):1621-42.
- Baehr M, Frotscher M. Duus’ Topical Diagnosis in Neurology: Anatomy, Physiology, Signs, Symptoms
. Fourth Edition. Stuttgart: Thieme, 2005.
- Nolte J. The Human Brain: An Introduction to its Functional Anatomy
. Sixth Edition. Philadelphia: Mosby, 2008.
- Greenberg MS. Handbook of Neurosurgery
. Sixth Edition. New York: Thieme, 2006. Chapter 25.