Head CTs are a common, inexpensive, and fast way of evaluating intracranial pathology. Although they do not give the anatomical detail of an MRI, they are still extremely important in diagnosing “gross” pathology that needs emergent intervention.
CT scans are based on the Hounsfield unit (HU), which is an indirect way to measure density. Interestingly, Sir Godfrey Newbold Hounsfield won a Nobel prize for his work on developing the CT scanner, but I digress…
The importance of the Hounsfield unit is that things that are hyper-dense (very dense) appear bright; those things that are hypo-dense (not very dense) appear dark. The different tissues and fluids within the confines of the skull have varying densities. The most dense materials, like bone, have very high Hounsfield units; less dense materials such as air and cerebrospinal fluid have very low Hounsfield units.
It is important to approach head CTs in a systematic fashion so that subtle (and not so subtle) pathology is not missed. The easiest way I have found to read a head CT is to remember the following mnemonic:
Blood Can Be Very Bad
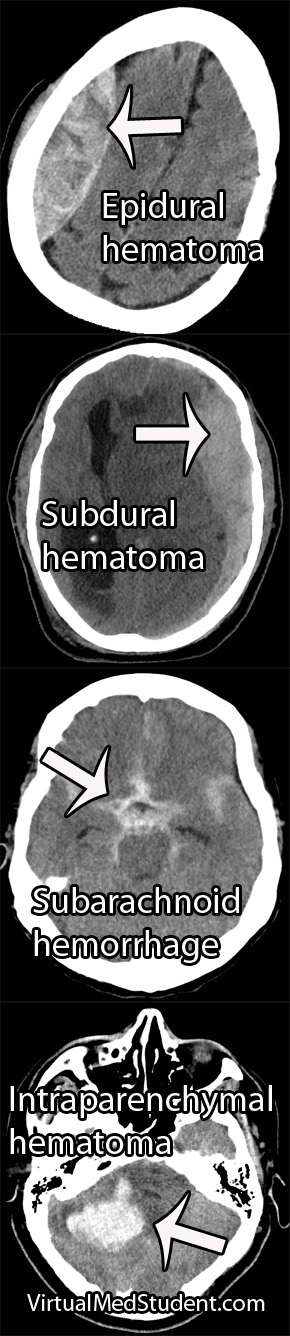
The first “B” in the mnemonic stands for, you guessed it, blood. There are five different pathological locations that blood can be located: epidural, subdural, subarachnoid, intraventricular, and intraparenchymal. Depending on the age of the blood, it may be hyper-dense (acute/active bleeding), isodense (roughly 3 to 7 days old), or hypo-dense (older than 7 days).
The second "B" stands for "brain". Although blatant pathology such as blood clots are usually readily apparent, more subtle pathology can also be obtained from a CT. For example, blurring of the gray-white junction may indicate evolving stroke. Any areas of hypodensity (ie: dark areas) within the brain may indicate edema associated with a tumor.
The "V" represents the ventricular system. The ventricular system consists of a pair of lateral ventricles, a third ventricle, and a fourth ventricle (don’t ask me what happened to the first and second ventricle!). The ventricles are in communication with one another via holes known as foramen. The paired foramen of Monroe connect the lateral ventricles to the third ventricle; the cerebral aqueduct of Sylvius connects the third ventricle to the fourth ventricle. The fourth ventricle drains into the subarachnoid space surrounding the spinal cord via the foramen of Magendie and Lushka.
The ventricular system is quite symmetric. Any obvious asymmetries may indicate a pathologic process "pushing" on a ventricle causing it to become distorted. In addition, if the ventricles are larger than normal it may indicate the presence of hydrocephalus, a condition in which cerebrospinal fluid is not reabsorbed appropriately.
The final "B" in the mnemonic stands for "bone". The skull should be assessed for fractures, especially in trauma patients. A common place for fractures is at the skull base. Time should be spent assessing this area to rule out fractures that extend across the canals and foramen that house the carotid arteries, jugular veins, and cranial nerves.
Reading a head CT is the first step in determining what additional imaging studies are necessary, or what treatment should be given. By using the above mnemonic it allows the interpreter of the scan to quickly and effectively assess if there is underlying pathology that needs further evaluation.
Overview
The mnemonic – blood can be very bad – can be used to systematically interpret a head CT. The first "B" stands for blood. The "C" stands for cisterns. The second "B" stands for brain. The "V" represents the ventricular system. And the last "B" stands for bone. By looking at these five components it is possible to assess all the important pathology that may require further imaging and/or treatment.
References and Resources
- Park JH, Park YS, Suk JS, et al. Cerebrospinal fluid pathways from cisterns to ventricles in N-butyl cyanoacrylate-induced hydrocephalic rats. J Neurosurg Pediatr. 2011 Dec;8(6):640-6.
- Baehr M, Frotscher M. Duus’ Topical Diagnosis in Neurology: Anatomy, Physiology, Signs, Symptoms
. Fourth Edition. Stuttgart: Thieme, 2005.
- Frontera JA. Decision Making in Neurocritical Care
. First Edition. New York: Thieme, 2009.
- Greenberg MS. Handbook of Neurosurgery
. Sixth Edition. New York: Thieme, 2006. Chapter 25.